Pancreatic Cancer
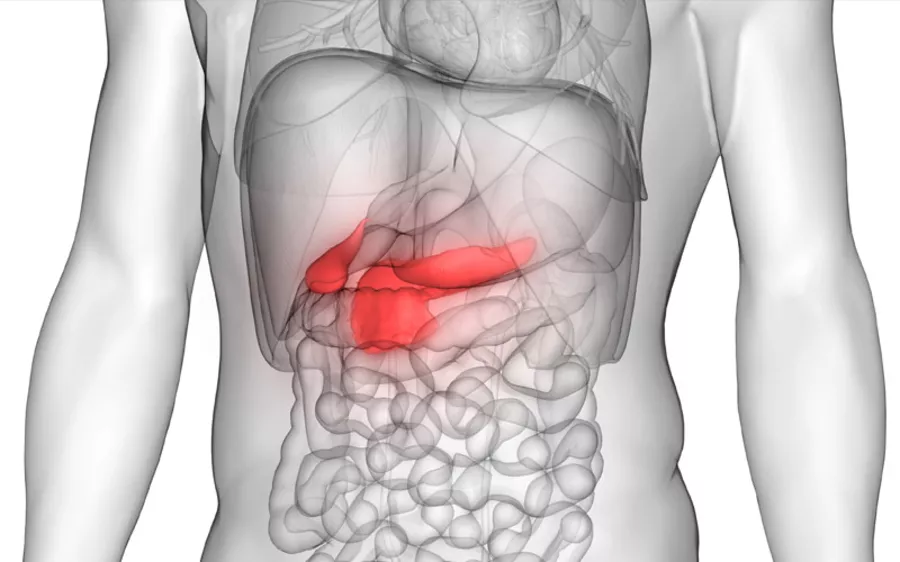
Pancreatic cancer begins in the tissue of your pancreas, which is an organ that lies behind the lower part of your stomach. Your pancreas secretes enzymes and hormones that are important for digestion - it breaks down sugar and other nutrients, helping you absorb them and controlling your blood sugar levels.
The most common type of pancreatic cancer is adenocarcinoma. This accounts for 95% of all cases. A few cancers originate in pancreas cells that make hormones. These are called neuroendocrine tumours.
Typically cancer of the pancreas spreads quickly, which can make it difficult to treat.
In more detail
Most commonly, pancreatic tumours begin in the organ’s lining and are known as exocrine pancreatic tumours, or adenocarcinoma. These tumours account for 95% of all cases.
There are two common types of exocrine pancreatic tumours. Those that start in the ducts of the pancreas are called ductal adenocarcinoma. Much less commonly, a tumour can begin in the acini, which are parts of the pancreas that connect to the ducts. These are called acinar adenocarcinoma.
Rarer exocrine pancreatic tumours include: acinar cell carcinoma, adenosquamous carcinoma, colloid carcinoma, giant cell tumour, hepatoid carcinoma, mucinous cystic neoplasms, pancreatoblastoma, serous cystdenoma, signet ring cell carcinoma, solid and pseudopapillary tumours, squamous cell carcinoma, and undifferentiated carcinoma.
Making up the remaining 5% of pancreatic cancer are tumours that originate in the islet cells of the pancreas, called Islet cell carcinoma or neuroendocrine tumours. Islet cells make hormones like gastrin, insulin, and glucagon. Tumours that cause the islet cells to overproduce these hormones are known as functional tumours. They can cause symptoms such as low blood sugar, diabetes, skin rashes, gallstones, stomach ulcers and diarrhoea. Tumours that do not affect the islet cells hormone production are called “non-functional” and most are malignant.









