Breast Cancer
Breast cancer is the most common cancer for New Zealand women.
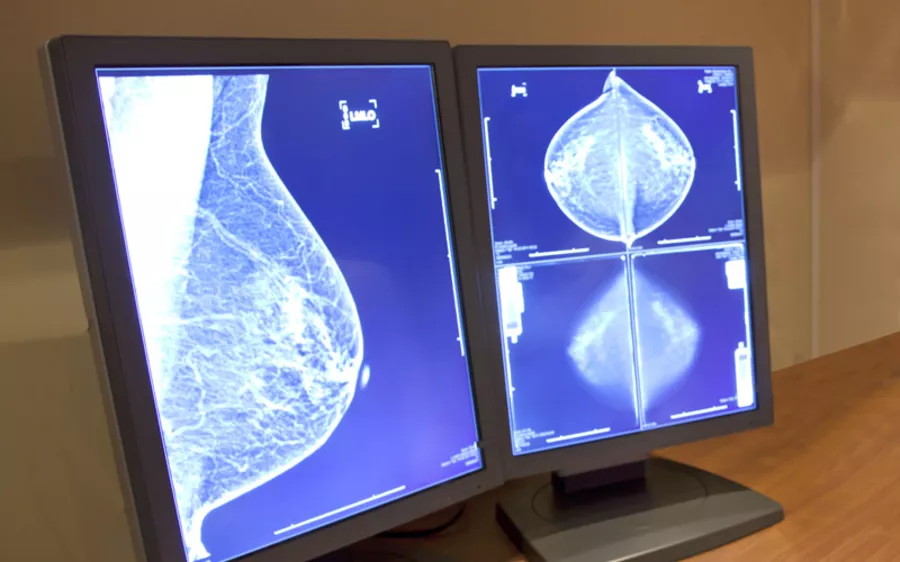
What is breast cancer?
Breast cancer is when abnormal cells in the breast begin to grow and eventually form a growth (tumour) which can spread within the breast or around the body. Breast cancer can develop over several years.
Signs and symptoms of breast cancer
There may be no warning signs that you have breast cancer. Some signs and symptoms may include:
- A new lump in the breast
- Nipple discharge
- Changes in the nipple, such as turning inwards, ulcers, persisting redness
- Changes in the breast such as shape or size or changes on the skin of the breast such as skin dimpling, redness
- Pain in the breast that doesn't go away
Although these symptoms can be caused by conditions other than cancer, it's important to get them checked by your doctor as soon as possible.
Types of breast cancer
Nearly all breast cancers are carcinomas, which is a cancer that begins in the epithelial cells of organs like the breast. The ducts and lobules of the breast are glandular tissues. Glandular tissues make and secrete a substance, such as milk, and cancers starting here are often called adenocarcinomas.
If the breast cancer has stayed in the ducts or the lobules, and the cells have not invaded the rest of the breast or spread to other parts of the body, this is called ductal carcinoma in situ or lobular carcinoma in situ. Sometimes it is referred to as non-invasive or pre-invasive, because it might develop into invasive cancer if left untreated.
Breast cancer that has already grown beyond the layer of cells where it started, is known as infiltrating carcinoma or invasive carcinoma. Most breast cancers are invasive carcinomas and are either invasive ductal carcinoma or invasive lobular carcinoma.
Sarcoma are cancers that start in connective tissues such as muscle tissue, fat tissue, or blood vessels. Sarcomas of the breast are rare.
For more information on types of breast cancer, visit: Types of breast cancer (NZ Breast Cancer Foundation)
Stages of breast cancer:
Every breast cancer diagnosis is given a stage and a grade. These, along with the type of cancer, help to determine what treatment is best. Breast cancer stage refers to how big the cancer is and whether it has spread.
Breast cancer grade refers to what the tumour looks like in comparison with normal cells, which helps determine how quickly the cancer is growing and how it might behave.
For more information, visit: Breast cancer staging
Radiation treatment for breast cancer
Radiation therapy, also known as radiotherapy, uses high-energy x-ray beams to destroy or control the growth of cancer cells by damaging their DNA.
This is a targeted treatment, focusing only on the specific area requiring therapy. While some healthy tissue may be exposed, it typically has the ability to repair itself—unlike cancerous cells.
In cases of early breast cancer, radiation therapy is commonly used after breast-conserving surgery (such as a lumpectomy or partial mastectomy) to eliminate any remaining malignant or pre-cancerous cells. This significantly lowers the risk of cancer returning in the treated breast. It may also be recommended after a mastectomy when certain high-risk features are present.
Treatment may also extend to regional lymph nodes, such as those in the underarm (axilla), above the collarbone (supraclavicular area), or along the internal mammary chain (near the breastbone), depending on the clinical situation.
Extensive international research has shown that radiation therapy in these contexts reduces the likelihood of cancer recurrence in the breast.
Typically, radiation therapy is started after surgery once healing is complete. If chemotherapy is also required, radiation usually follows the completion of that treatment.
Radiation treatment of the breast is undertaken with a treatment machine called a linear accelerator, which delivers radiation beams from outside the body, targeting the whole breast or chest wall. Whole Breast Radiation Therapy is delivered daily (five days a week, excluding weekends, to allow the healthy cells to recover), and can be delivered in as little as five days, with a maximum of twenty days. The number of treatments you will receive is dependent on a number of factors and will need to be determined by your Radiation Oncologist.





















